Digestive system >>>> Nutcracker's esophagus
Nutcracker's esophagus.

The Nutcracker's esophagus or the common name in the medical literature is segmental esophagospasm (from the Latin "oesophagus" - esophagus), belongs to the number of esophageal dyskinesias, or rather, hypomotor disorders of the esophagus. In modern literature, one can find another name for segmental esophagospasm - Barsoni-Taschendorf syndrome (" rosary-figurative esophagus " from the word "rosary"). This name was inspired by its author by the appearance of segmental esophagospasm seen on the radiograph.
Regarding the classification of this disease as a group of functional diseases of the esophagus , it is believed that dyskinesias of the esophagus are persistent disorders of esophageal motility (there are still unstable, transient spasms of the esophagus, which can be observed in healthy people during stress or swallowing poorly chewed food - in large chunks)
The causes of the Nutcracker's esophagus have not yet been fully studied, but it is safe to say that the development of this disease is observed against the background of certain diseases: peptic esophagitis, hiatal hernia, parkinsonism, bronchial asthma and others.
There is also an opinion that the causes of segmental esophagospasm are a consequence of psychosomatic disorders: depression, hysteria. And, finally, persistent esophagospasm can be the result of short-term, but periodic nervous shocks .
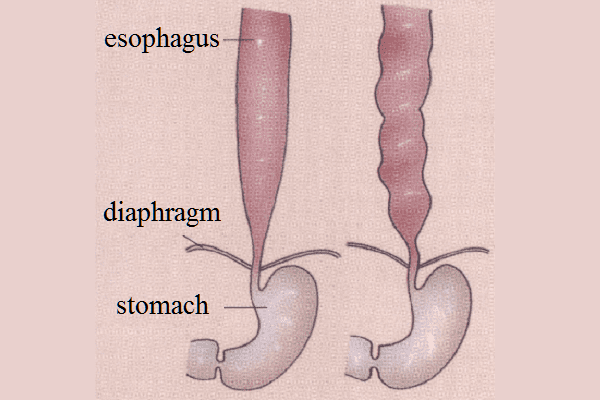
A significant advance in the analysis of the causes of the Nutcracker esophagus and other hypomotor disorders of the esophagus was made by the discovery of certain biologically active substances of a hormonal nature. Endorphins, enkephalins, somatostatin, thyrotropin and other substances were found in the tissues of the brain, which were also identified in the organs of the digestive system. This made it possible to speak about the existence of a certain informational cellular system - the diffuse endocrine system of Fairter (also called “APUD - Pierce's system” ). That is, in fact, a direct endocrine connection between the central nervous system and the digestive system was discovered.
The essence of esophagospasm is a violation of the peristalsis of the esophagus in its various parts. When they talk about segmental esophagospasm, they mean that disruptions in peristalsis occur in small areas of the esophagus (segments), and not along its entire length. The amplitude of oscillations of the esophageal wall in these areas increases (more than 180 mm Hg). There can be many such segments, and then one speaks of multiple segmental contractions, but these contractions are stable. Such failures allow the food bolus to move, but the person is in pain.
Nutcracker esophagus signs.
- Dysphagia (violation of the swallowing process) - food passes, but pain occurs.
- Feeling of heaviness behind the breastbone.
- Retrosternal pain (not typical) - radiating to the shoulder, neck, epigastric region and even the lower jaw; may disappear by drinking warm liquid.
- Heartburn, belching, vomiting - observed with a combination of segmental spasm of the esophagus and insufficiency of the cardia (esophageal sphincter muscle) of the esophagus.
- May be asymptomatic (20% of cases).
Diagnosis of esophageal spasm .
Diagnostics of the Nutcracker's esophagus is carried out in two directions: firstly, differential diagnosis is carried out with diseases that have similar symptoms, for example, with angina pectoris. There are times when chest pain occurs in the morning and is well removed by nitroglycerin, which misleads the doctor. There are cases when angina pectoris begins against the background of esophageal spasm (that is, it develops as viscero-visceral reflexes). In these cases, angina pectoris can be excluded only with the help of thorough hardware studies, which constitute the second direction in the diagnosis of esophageal spasm.
Hardware diagnostics include:
- X-ray of the esophagus, which reveals spastic contractions of areas of the esophagus, and makes it possible to visualize them.
- Endoscopy of the esophagus to exclude organic changes in the tissues of the esophagus causing dysphagia.
- Esophageal manometry to analyze the nature of spastic movements of the esophageal wall.
- Ultrasound diagnostics of the esophagus , which examines the motor and sensory functions of the esophagus and makes it possible to differentiate segmental esophagospasm from diffuse.
Nutcracker Esophagus Treatment.
The essence of the treatment of esophageal spasm is symptomatic and boils down to the following:
Removal of smooth muscle spasm or decrease in the amplitude of oscillations and relief of pain syndrome:
- Drinking warm liquids
- Antispasmodics
- Cholinomimetic and anticholinesterase agents
When esophageal hypomotor dyskinesia is combined with insufficiency of the lower esophageal sphincter, antispasmodics and anticholinergics are not used, since these drugs affect the enhancement of gastroesophageal reflux.
- Calcium channel blockers.
- Nitrates - not helping in all cases.
- Botulinum toxin injections (temporary effect).
- Proton pump inhibitors (when combined with gastroesophageal reflux.
- Sedatives and antidepressants (in difficult cases).
Organization of the correct meal:
- Crushing and chewing food thoroughly
- Alternating dry food with liquids during meals
- A leisurely meal
- While eating, do not be distracted by watching a movie, reading a book, or talking.
Complications and prognosis of segmental esophageal spasm.
Complications of dyskinesia are considered in the form of the development of other diseases of the esophagus: hypermotor disorders of the esophagus, hiatal hernia, esophageal diverticula, esophageal stricture. But with targeted and persistent treatment, the prognosis is considered favorable if esophageal dyskinesias did not initially have concomitant diseases (in this case, concomitant diseases are treated in parallel).

Read

Read